Challenges in vaccine rollout linked to cooling
Approximately 2.7 billion people would lack dependable access to vaccines as a result of insufficient supply chains and logistics capabilities related to cold chains.
Even though supply challenges are the primary vaccine delivery constraint, the scale of the cold chain challenge to reach herd immunity, even at conventional storage temperatures between 2°C to 8°C, is still immense and has exacerbated existing cooling access gaps and created new ones. The herd immunity threshold for COVID-19 has been estimated to be at least 60–70 percent, which translates into 4.7 to 5.5 billion people.
Challenges could also persist if, given the emergence of mutations and unknowns on the longevity of immunity, regular booster shots are required over time. India has one of the world’s largest routine immunization programmes targeting 29 million pregnant women and 26.7 million newborns every year, yet this is far from the scale needed to immunize India for COVID-19. [13]
The inequalities between richer and poorer nations in vaccine distribution are clear, including secured vaccines and cold chains needed to distribute the vaccines. Ellen Johnson Sirleaf, the former President of Liberia and current Co-Chair of the Independent Panel for Pandemic Preparedness & Response (IPPR) recently expressed her disappointment that based on current plans, vaccines would not be widely available in Africa until 2022 or 2023. Similarly, the Economist Intelligence Unit forecasts that 85 poor countries will not have widespread access to COVID-19 vaccines before 2023, including all African countries with the exceptions of Egypt, Ethiopia, Gabon, Kenya, Morocco and South Africa. [14]
Temperature control and vaccine cold chains are certainly a key contributing factor. A recent DHL logistics study concluded that even with conventional cold storage requirements, the proportion of the world’s population with good access to a vaccine, based on available logistics and supply capabilities, would only be about 70 percent. On this basis, approximately 2.7 billion people would lack dependable access to vaccines as a result of insufficient supply chains and logistics capabilities related to cold chains. [15]
Health facility electricity access
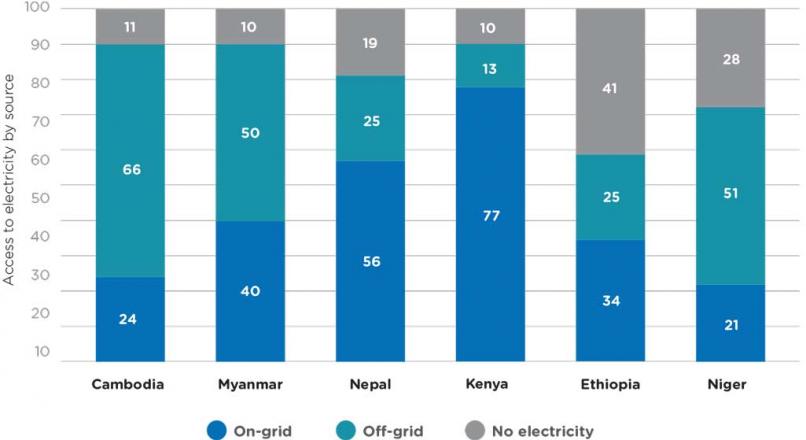
The World Bank surveyed 730 health facilities in six countries (Cambodia, Ethiopia, Kenya, Myanmar, Nepal and Niger) under its Multi-Tier Framework (MTF) approach in 2013. Off-grid solutions can be sufficient provided there is enough capacity, and moreover the surveys also highlight that approximately 25 percent of health facilities lack a primary source of electricity, in line with estimates from previous studies (Figure 3.2). Additionally, the surveys showcase significant differences between countries, with half or more of health facilities in Cambodia, Myanmar and Niger relying on an off-grid power solution. The surveys also highlight that grid power does not always equate to quality and reliable electricity, with 25 percent of surveyed on-grid health facilities reporting outages that affect health facilities’ ability to offer health services. Unreliable power and voltage surges contribute significantly to equipment breakdown and can cause vaccine losses with associated human health implications.
Figure 3.2: Electrification of health institutions in select MTF countries, by source (2013)
Sub-Saharan Africa
In Sub-Saharan Africa, where vaccine cold chain challenges are significant, reliable energy access in hospitals and clinics is a key need. Long before the COVID-19 pandemic made daily headlines, a lack of reliable power in healthcare facilities was undermining the quality of healthcare for millions of people in Sub-Saharan Africa. While data on the size of the energy access gap in the health sector are sparse, a handful of multi-country studies all point in the same direction. A 2013 WHO-led review in 11 countries in Sub-Saharan Africa estimates that one in four health facilities had no access to electricity at all, [16] while only 28 percent of health facilities and 34 percent of hospitals were considered to have ‘reliable’ electricity. A different study [17], focusing on ‘reliability’ of electricity in health facilities in low- to middle-income countries, estimates that 59 percent lack reliable electricity that would be necessary to power vaccine storage appliances that must be connected to electricity. Globally, the International Renewable Energy Agency (IRENA) has estimated that approximately 1 billion people rely on health facilities that have no electricity supply. [18]
To address challenges related to electricity access and power fluctuations that can impact the efficacy of vaccine refrigerators, Gavi has been engaged in the procurement of 65,000 off-grid-ready, solar direct-drive refrigerators for nearly 50 countries and is now prioritizing them for last-mile vaccine delivery. To support the vaccine rollout under COVAX, in late 2020, UNICEF began purchasing 92,000 vaccine fridges, 11,325 of them solar-powered, as well as cold boxes and vaccine carriers. [19]
Such solutions are relatively expensive but are good in areas with limited energy access and help replace reliance on diesel. Portable cold boxes and refrigerated vans are other solutions that can support countries in reaching the last mile. Innovative business models can also make these solutions more accessible, in particular pay-as-you go (PAYG) models for technologies previously deployed in the agricultural cold chain.
The World Bank Group has made a USD 12 billion financing envelope available to developing countries to support the purchase of vaccines and strengthened health systems, including cold chains. One of the first approved projects provided support to Cabo Verde to purchase and deploy vaccines for 35 percent of its population, which included the financing of cold chain equipment and transport. [20] Similarly, the World Bank’s Energy Sector Management Assistance Program (ESMAP) also provides technical and investment support for reliable and climate-friendly health facilities and vaccine cold chains in Sub-Saharan Africa.